The Sex Talk: How to avoid getting pregnant if you're not ready yet
Editor's Note: We believe that virginity, birth control, and sex are still opaque topics here in the Philippines. A discussion about these things with our parents mostly involves them telling us never to have intercourse or get pregnant until we're married. However, that is hardly a deterrent for women to make unwise choices. At Project Vanity, our ultimate goal is to empower women by providing them information about their own bodies so they feel more confident navigating their world.
In The Sex Talk, a new section here at PV, we aim to consult with doctors and experts about common questions we feel should be answered by women, for women.
Sex isn't evil nor should it be a taboo topic. If you're sexually active, you shouldn't be ashamed of using your body in a manner that makes you happy. If you're not sexually active, that's cool too. It's your body and you have the right to decide what to do (or not to do) with it.
You do, however, have to be responsible for your choices. For instance, it's important to know how to avoid getting pregnant if you're not ready to raise a child. What if your boyfriend isn't into condoms? Do you put complete faith in his ability to withdraw before he ejaculates?
Often, birth control is a woman's burden. That's why we’re taking a closer look at artificial birth control methods currently (and legally!) accessible to Filipinas.* With the expert medical advice of Dr. Cecilia Vicencio, head of the Department of Obstetrics and Gynecology at The Medical City, we are here to give you a rundown of your options and what you really need to know if you wish to avoid pregnancy for the meantime.
While we hope this helps you decide on which method is best for you, it should not be taken as a substitute for medical advice as your doctor will be better able to evaluate your particular needs.
What women want
When asked to name the most popular artificial birth control methods among Pinays, Dr. Vicencio tells us that the Combined Oral Contraceptive Pill (COCP) is still the go-to. This is followed by injectables and intrauterine devices (IUDs). Surprisingly, the lowest on the list was male condoms!
Considering how easy it is to purchase condoms in drugstores, groceries, and pretty much anywhere, we were shocked that it was the one least preferred. It doesn’t even make the Top 3. The doctor explained that male partners usually complain that condoms feel thick and can cause a loss of sensation. Yep, even when using ultra-thins! When it comes to preventing sexually-transmitted diseases though, condoms are the only option, as they form a physical protective barrier. Unfortunately, female condoms are not available in the PH.
As for the birth control patch (which was launched only a few years ago), it didn’t enjoy much success locally due to its high price. So while it’s technically available, it’s pretty hard to find and isn’t considered a cost-effective solution. For this feature, we decided to just focus the discussion on the top three most preferred methods. Most of the contraceptives discussed here contain synthetic hormones that essentially keeping you from ovulating, thereby preventing the development and maturation of an egg cell. The hormones also cause the cervical mucus to thicken, so sperm can’t properly swim “upstream” to the vaginal area.
The Pill
Combined Oral Contraceptive Pills (COCPs) can be broken down into two main types: the progestin-only pills and the combination pills. Progestin is a hormone that suppresses ovulation, and it can be taken alone or combined with estrogen. There are different types of progestin, which is why there are lots of different pill formulations, and these are typically prescribed for breastfeeding women (as estrogen in combination pills can suppress lactation.)
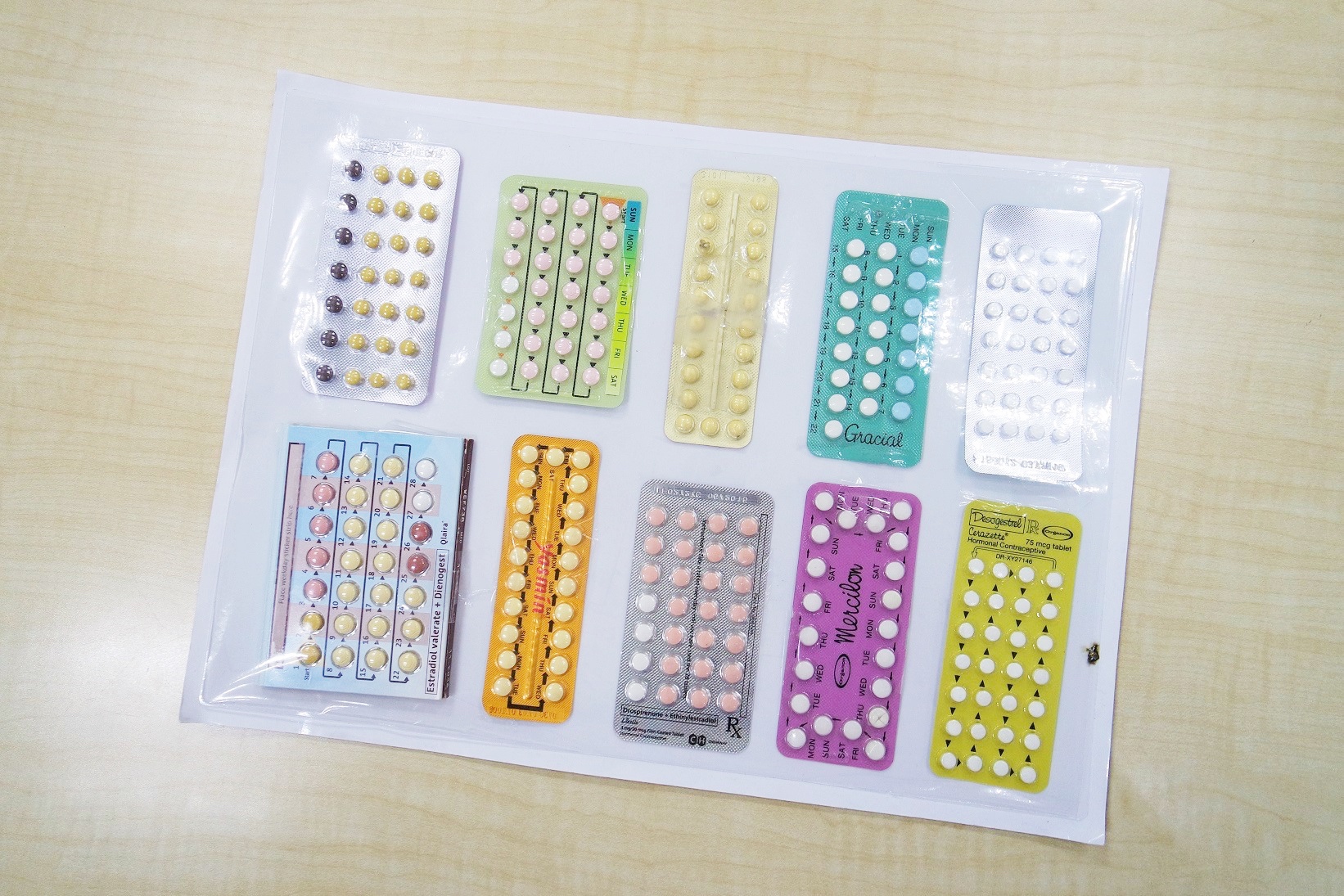
Aside from formulations, different brands of pills will vary in terms of the number of active and inactive/blank pills. Some have the user stop for a few days every cycle to allow her “menstruate” (only the uterine lining is shed as there are no eggs released) while other types must be taken daily to maintain the routine of taking them regularly. For example, Brand X has 24 active pills and 4 inactive ones to complete the 28-day cycle, whereas Brand Y has 21 active pills and 0 inactive pills that require the user to stop taking pills for the remaining 7 days.
Finding the right pill formulation for you requires your doctor’s prescription so please only take pills under their supervision! If you experience adverse reactions, it may mean that you need to use a different pill and your doctor can prescribe a new formulation. The success rate for contraceptive pill use is 91%.
The Good: Some formulations of combination COCPs like Cyproterone Acetate have the added bonus being anti-acne! This is why the Pill is sometimes prescribed by dermatologists as an acne treatment. You can also stop at anytime should you want to try getting pregnant.
The Bad: Smokers and those with a history of hypertension, heart problems, diabetes, and deep vein thrombosis are not recommended to take the Pill as they can increase blood pressure and worsen circulatory problems.
Injectibles
For those who just can’t seem to follow the stringent daily schedule of remembering to take the Pill, a depo medroxyprogesterone acetate (DMPA) shot is the next best option. It’s more popularly known by its brand name, Depo-Provera, and functions in pretty much the same way as the progestin-only Pill does. A single dose is enough to cover you for three months though so you don’t need to worry about taking a pill everyday. It also has a higher success rate at 94%.
The Good: A little bit goes a long way! At just over P100 per shot, DMPAs are actually quite affordable in addition to being convenient.
The Bad: It’s a no-go for those who are uneasy with the prospect of being pricked with a needle, and for those who might not want to wait three months to be able to get pregnant.
IUDs
For those who have yet to see an intrauterine device in real life, it might come as a shock that it’s actually a really tiny piece of T-shaped plastic with a copper wire snaking around it. “The copper works as an irritant, inducing an inflammatory changes [within the uterus] that destroys sperm,” explains Dr. Vicencio. Some IUDs are also designed to contain and gradually release progestin. The hormones inhibit ovulation and thin the lining of the uterus. At just slightly bigger than a 5-peso coin, a doctor positions it into the uterus, and the device can stay there for up to three years (or more) before replacement is required. At 99%, this is also the most reliable contraceptive option available.
The Good: If positioned properly, you wouldn’t be able to feel anything, except perhaps for the string that hangs outside the cervix. It stays effective for a very long time and should you decide to start trying for a baby, you can just have it removed and your fertility will be easily restored.
The Bad: The string on the IUD can be quite problematic as it tends to make you more prone to infection. Also, those who use tampons must be careful not to pull out the IUD string along with it.
What you should know
While your OB-GYN may have explained how your choice of contraceptive works and how to properly use it, you may have missed a few things in this rather lengthy discussion. We asked Dr. Vicencio about the most common misconceptions about contraceptives, and we’re debunking them, STAT!
Myth 1: There’s ZERO chance of getting pregnant if you’re using contraceptives.
Even though the top 3 methods are immediately effective and may even offer long-term protection, none of them are completely infallible. “No contraceptive is 100% effective. There’s always a 1-2% chance of getting pregnant,” explains Dr. Vicencio.
Myth 2: When you stop taking the Pill (as part of the cycle) or when you take the placebo ones, you menstruate.
Um… Not really. What comes out isn’t “real” menstruation! The hormones prevent ovulation to begin with, so your ovaries don’t release any eggs that can be fertilized or menstruated out as usual. What actually happens is called “breakthrough bleeding” and what comes out is just remnants of the uterine lining. This is why “periods” are usually lighter when on the Pill.
Myth 3: You need to menstruate to “clean out” your uterus.
Since there is no egg cell to drop, there is nothing to clean. “Menses are not something that you need to have to expel toxins,” emphasizes Dr. Vicencio. “You’re not going to menstruate if you don’t ovulate.”
Myth 4: Artificial hormones in contraceptives can cause permanent infertility or birth defects later down the line.
Not at all! According to Dr. Vicencio, “When you stop taking the Pill, there will be breakthrough bleeding. But after that and you get your period normally the following month, the Pill will have completely lost its effect. You can regain fertility almost immediately.” And since the Pill no longer works, it won’t affect the embryo once the pregnancy begins.
We hope this sheds light on some of those burning questions! And remember: it’s always important to be in tune with your body’s needs. Always be honest with your OB-GYN about your experiences and medical history so that they can prescribe the best option for you. Let them know if you feel uncomfortable so they can re-evaluate your contraception.
*We will publish another story on natural birth control methods.
Sources: Rappler, Broadly, PSA,
Header image via netdoctor.co.uk